What Has Covid-19 Taught Us about Strengthening the DOD’s Global Health Security Capacities?
Thomas R. Cullison and J. Stephen Morrison. "What Has Covid-19 Taught Us about Strengthening the DOD’s Global Health Security Capacities?." CSIS Commission on Strengthening America's Health Security, Center for Strategic and International Studies, May 11, 2021. Accessed October 01, 2025. https://healthsecurity.csis.org/articles/what-has-covid-19-taught-us-about-strengthening-the-dod-s-global-health-security-capacities/
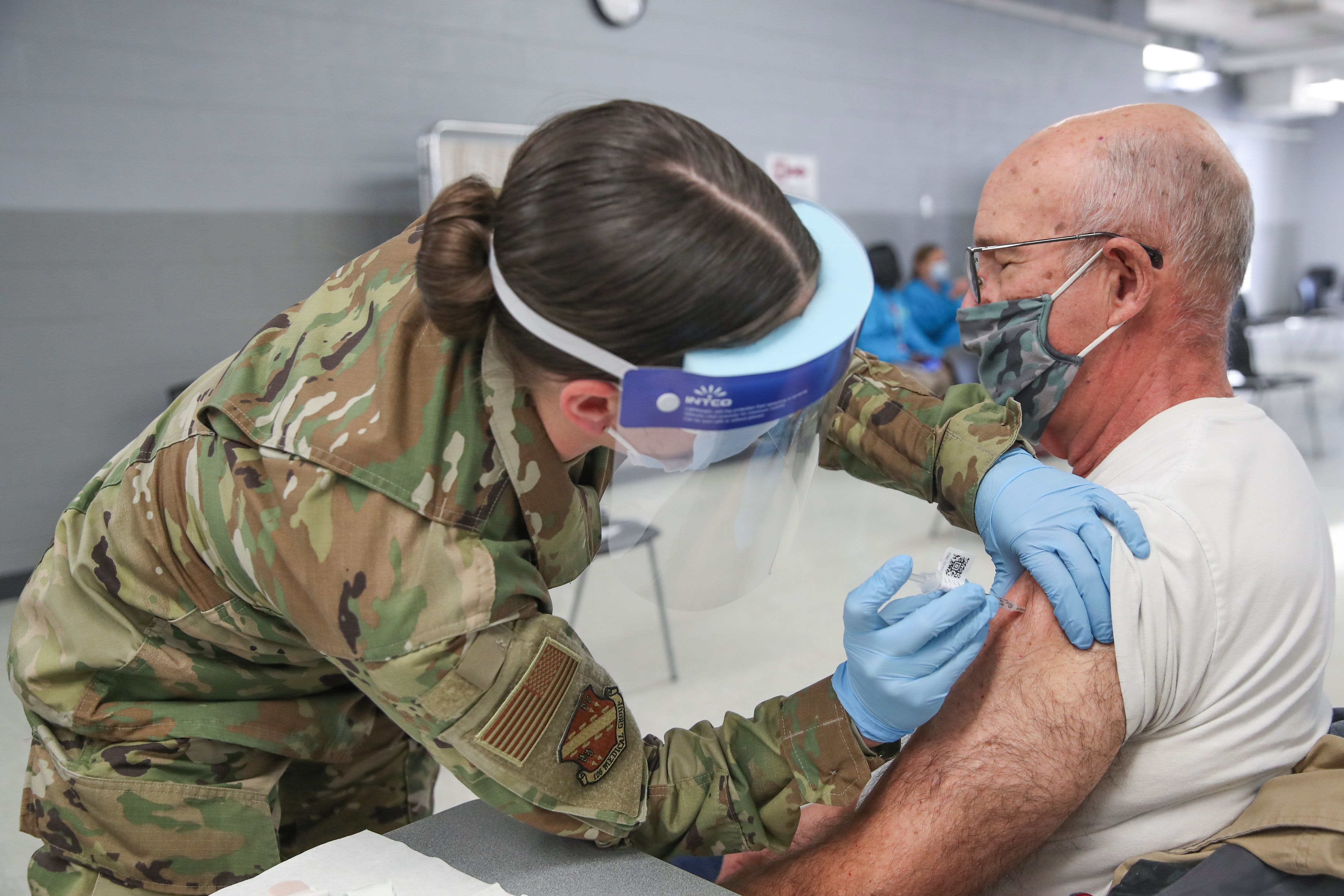
The Covid-19 pandemic has led to millions of deaths and cases of enduring illness, destabilized economies, diminished U.S. international standing, and exposed the U.S. military to challenges not experienced in over a century. Since the pandemic began, the U.S. Department of Defense (DOD) has been heavily involved in addressing challenges to the armed forces while supporting the overall national Covid-19 response.
Future biological threats will undoubtedly present new challenges. Yet broad U.S. military expertise in health, biosecurity, and biosafety will continue to contribute substantially to coordinated, interagency global health security efforts. Below are five recommendations for how the Biden-Harris administration and members of Congress can help steer impending deliberations over the future of the DOD’s contributions to global health security. As U.S. diplomatic engagement expands to address the worsening vaccine crisis and other related global health security challenges, there will soon be increased calls for the DOD to contribute in new and important ways that draw on its exceptional logistics, planning, lift, and scientific capacities. These recommendations are meant to complement the excellent and extensive recent analysis by Mark Cancian and Adam Saxton of the CSIS International Security Program on how the U.S. military responded to Covid-19 to guarantee the protection and readiness of U.S. forces and how it supported the civilian pandemic response at home. That study and this white paper are both part of the work of the CSIS Commission on Strengthening America’s Health Security.
Broad U.S. military expertise in health, biosecurity, and biosafety will continue to contribute substantially to coordinated, interagency global health security efforts.
#1: Elevate Biological Threats
In the face of the pandemic, DOD leadership, in close consultation with the White House and Congress, should push for a fundamental change to the 2022 National Defense Strategy and the Defense Planning/Programming Guidance to codify the DOD’s role as a major interagency biosecurity partner in combating biological threats, whether naturally occurring, accidental, or intentional.
The DOD must decide whether to consider biological threats as adversaries or merely operational constraints. This depends in large part on whether senior leadership concludes that infectious diseases are indeed an ever-present national security threat. The 2018 National Defense Strategy (NDS) mentions biological threats only in the context of weapons of mass destruction, biological weapons, and bioengineering. Yet outbreaks from naturally occurring, accidental, and intentional sources are just as important—and the SARS-CoV-2 virus, which has caused the greatest number of casualties since World War II, has demonstrated beyond any doubt that unforeseen pathogens can rapidly undermine U.S. national interests if not detected and mitigated effectively. As the next step for senior policymakers, the 2022 NDS should declare unequivocally that biological threats, regardless of source, are national security risks and codify the DOD’s role as a major interagency biosecurity partner. That declaration should be followed up with clear budgetary and policy support.
#2: Protect and Strengthen Operational Assets
Senior policymakers at the DOD, the White House, and Congress need to have a far better understanding of what assets the DOD brings to the table in any consideration of U.S. approaches to global health security at home or abroad. This includes protecting and preserving its exceptional institutional capacities—its integrity, budgets, and leadership—and taking required steps to strengthen performance and usher in the next phase of innovation. These assets, of high importance to addressing infectious disease threats, are fundamental to the readiness of U.S. troops. At the same time, they bring considerable depth and shared value to civilian-led health security efforts and to research and capacity-building partnerships with national governments, universities, and international organizations.
The most significant DOD institutions in biological research, public health, and biological surveillance infrastructure include:
- The Defense Advanced Research Projects Agency (DARPA), which works closely with other government agencies and partners in industry and academia to explore molecular biology, artificial intelligence, and other emerging fields to develop measures for countering disease.
- The Defense Threat Reduction Agency’s Biological Threat Reduction Program (BTRP), which facilitates the detection, surveillance, security, and elimination of especially dangerous pathogens.
- Overseas Army and Navy infectious disease research laboratories, the Global Emerging Infections Surveillance (GEIS) system, the military services’ preventive medicine units, and other organizations that continually address militarily relevant infectious disease threats. These form the core of an extensive military infectious disease surveillance network that collaborates with the U.S. Centers for Disease Control and Prevention (CDC) and the World Health Organization.
- The Uniformed Services University of the Health Sciences (USUHS), which compiles Covid-19 treatment strategies and techniques into regularly updated and publicly available practice management guidelines.
- The National Center for Medical Intelligence, a resource for information on biological agents of all types.
Examples of recent achievements include military laboratories at home and overseas conducting foundational basic science research on previous coronavirus outbreaks, notably severe acute respiratory syndrome (SARS) and Middle East respiratory syndrome (MERS). Beginning in early 2020, this progress by the DOD contributed significantly to rapid Covid-19 vaccine development. Much of the DOD’s ongoing biological preparedness efforts focus on diseases found mainly outside of the United States—such as malaria, dengue fever, Rift Valley fever, and Japanese encephalitis—that pose a risk to forces abroad, particularly in tropical areas. Military facilities have also developed biological threat detection tools that have become essential in warning against all types of biological exposure, such as from the anthrax letters sent to Congress following September 11, 2001.
It would be invaluable if DOD leadership reviewed each of these key remarkable assets in 2021–22 with an eye to strengthening their performance and leadership and putting them on a budgeting pathway that will lead to future innovation.
#3: Secure the Future of the DOD’s Medical Skill Base
The DOD’s contributions to health security at home and abroad rest overwhelmingly on the human skill base of the Military Health System (MHS). Yet that base remains vulnerable and fragile, specifically to budget decreases, reorganization, and staff cuts. Senior policymakers at the DOD, the White House, and Congress need to understand the true budgetary and retention requirements for sustaining the DOD’s remarkable professional skill base. This includes ensuring that proposed staff cuts and evolving plans for unifying health service delivery across the armed forces do not risk pushing out and discouraging the DOD’s career military medical professionals.
Dedicated people make an organization function. The DOD’s most valuable biosecurity and health assets are its highly skilled clinicians, researchers, and support staff. Its biosecurity and health professionals have been carefully recruited, educated, and trained to face the most pressing health challenges of today and the future. Training a single surgeon or infectious disease specialist from medical school to board certification takes a decade, and basic science researchers require similar timeframes to develop useful skills. Eliminating or weakening key skills would be like removing blocks in a Jenga tower—things will be stable for a time but may suddenly collapse.
The MHS is an integrated, worldwide health network with dual responsibilities of ensuring medical readiness and providing top-tier healthcare to over 9.6 million beneficiaries. Meanwhile, it deploys significant numbers of clinical and other staff for months at a time on short notice (including to civilian health systems for Covid-19 response), manages research and development institutions focused on military health threats and performance requirements, and operates worldwide disease and biothreat surveillance systems. MHS facilities also support training for military medical staff at all levels.
Although healthcare costs have risen rapidly across the United States, the DOD Unified Medical Budget has remained relatively flat over the past decade, currently $50.8 billion, or 7.2 percent of the Department’s $705.4 billion overall budget request for 2021.1 In comparison, overall U.S. healthcare costs have steadily increased, reaching 17.7 percent of GDP in 2019.
The DOD’s most valuable biosecurity and health assets are its highly skilled clinicians, researchers, and support staff.
What do these budget trends suggest? The DOD has kept the rise of its medical costs in check, demonstrating cost effectiveness year-in and year-out. But that has come at a price. Over the past decade, a relatively static budget has damaged morale and may have limited opportunities for medical providers to pursue critically important specialty training. The risk is that career medical staff increasingly hasten their departure from DOD ranks. Many of the Department’s best doctors in all specialties have remained in the military in order to teach and deepen their expertise. If denied these opportunities, they would likely leave to take up private-sector offers.
MILITARY HEALTH SYSTEM REORGANIZATION
Plans for MHS reorganization and proposed staff cuts will require particular attention to potential second- and third-order effects on recruitment and retention. Although much may be gained from consolidation and standardization, each potentially threatens to weaken DOD health and biosecurity capabilities in ways that may not be appreciated before it is too late to correct them, and it will be important to ensure unintended consequences do not lead to irreparable harm.
The National Defense Authorization Act for Fiscal Year 2017 (FY 2017 NDAA) mandated transitioning the administration and management of military treatment facilities (MTFs) to the Defense Health Agency (DHA)—though the military services retain control over operational medical requirements and functions, as well as installation-specific functions separate from MTF operations. This new framework has the advantage of allowing the services’ medical departments to focus on operational readiness missions while the DHA uses its authority, direction, and control over the MTFs to strengthen management of enterprise activities and make policies and procedures more efficient through standardization.
Many experts have raised concerns regarding the execution of the current transition plan. A 2020 Government Accountability Office report questioned assumptions regarding “support to the readiness of military primary care and non-physician medical providers,” among other concerns. In early August 2020, all service chiefs and secretaries took the highly unusual step of signing a memorandum to Secretary of Defense Mark Esper requesting the current transition plan be revisited, stating that “the proposed DHA end-state represents unsustainable growth with a disparate intermediate structure that hinders coordination of service medical responses to contingency operations, such as a pandemic.” However, Secretary Esper directed that the transition continue.
MILITARY MEDICAL FORCE REDUCTION
It is certainly important to ensure that the military medical force is appropriately sized and trained to address the DOD’s mission sets. Questions persist regarding the ability of the MHS to meet all mandates in the face of planned reductions of up to 17,000 military healthcare workers, or 20 percent of the current force. Fortunately, these plans were put on hold during the Covid-19 pandemic. Section 719 of the FY 2020 NDAA adds additional reporting requirements and delays for the DOD’s decision to realign military end strength and requires the Department to submit a report to Congress detailing medical personnel realignment. However, negative morale left over from previous cuts will likely worsen if these reductions are eventually reinstated.
All successful organizations must evolve to address future requirements, and certainly force-shaping considerations are appropriate. However, military medicine would be irretrievably decimated if consolidation and personnel cuts result in the closing of military graduate medical education (GME) programs or other military health education and training pipelines.2 These irreversible effects will not be realized for years.
Military physicians’ medical education is provided by both the USUHS Hébert School of Medicine and by U.S. civilian medical and osteopathic schools supported by the Health Professions Scholarship Program. Although the value of USUHS has repeatedly been questioned, the case for continuing to support and strengthen it remains compelling. Over the years, the retention rate of its graduates has been markedly higher than for those trained outside the DOD. It has contributed substantially to militarily relevant research, including on infectious disease, and has advanced professional education for military health professionals other than physicians.
#4: Launch a Military-to-Military Health Security Cooperation Initiative
The DOD should launch a signature initiative to promote military-to-military cooperation and build health security capacity among key partner countries. That effort should align with the broader U.S. diplomatic vision for shaping cooperative, coordinated action that will move countries out of the acute phase of the pandemic and prepare for the future. It will require buy-in from the White House and Congress, an implementation strategy, and sustained multi-year funding.
As the United States focused inward during the Covid-19 pandemic, other nations, notably China and Russia, have actively responded to the international demand for vaccines and medical supplies.
The Biden-Harris administration’s National Security Directive One (NSD-1) renews the United States’ commitment to leadership in multinational efforts to combat infectious disease threats. The opportunity exists to utilize and strengthen existing structures to meet these aspirations.3 In one positive step toward such national coordination, the new administration restored the National Security Council (NSC) position of senior director for global health security and biodefense.
As the United States renews its international leadership, it makes sense to include health and biosecurity efforts as a major part of national strategies for priority geographic areas, working with both individual nations and regional organizations. As the Biden-Harris administration develops its global health security strategy, it should incorporate a signature initiative on expanding military-to-military health security cooperation in support of broad U.S. partnerships with key allies in Asia and elsewhere.
As the United States renews its international leadership, it makes sense to include health and biosecurity efforts as a major part of national strategies for priority geographic areas, working with both individual nations and regional organizations.
For example, the Quadrilateral Security Dialogue (The Quad) between the United States, Australia, Japan, and India is an ideal forum for partnership on health and biosecurity issues in the Indo-Pacific region. This initiative should include expanded military-to-military cooperation to advance health security capacities among key partner countries in Asia and the Pacific, many of which have already reached out to the United States for access to vaccines, protective gear, and other critical commodities. The program could focus on staff training, management, preventive measures, data and surveillance, quick detection and contact tracing, and communications and community outreach. Such a program would require clear criteria for selecting countries and evaluating outcomes, new legislative authorities, and multi-year funding. It would build upon the DOD’s years of experience and existing capacities, as detailed in this report. Beyond public health, this would clearly meet a geopolitical need as well, with military-to-military cooperation serving as a soft power tool to further compatibility with like-minded militaries and counterbalance Chinese influence. Prospects for building bipartisan support for an initiative of this kind are promising, both in Congress and among the American people more generally.
#5: Transition Existing DOD International Health Engagement Activities into Sustainable, Integrated Programs
DOD leadership should more closely align the Department’s existing overseas health programs with a broader U.S. capacity-building strategy that builds out from the legacy of the Global Health Security Agenda. DOD overseas programs should transition from freestanding, siloed, episodic initiatives that are funded one year at a time to integrated efforts that have multi-year budgets.
A recent CSIS report states, “It is in the United States’ strategic interests to ensure that the world mobilizes effectively to end the SARS-CoV-2 pandemic. . . . These are fundamentally ethical, economic, and national security matters. Concerted U.S. action internationally will strengthen the protection of Americans at home but also lift the threat posed by the pandemic to the world’s most vulnerable populations, expedite the reopening of the global economy, and enhance U.S. influence in shaping solutions that align with U.S. values and interests.” The U.S. military can and should play a significant role in overseas health engagement, not only to control the current pandemic but also to advance international efforts to contain infectious diseases through closer collaboration with U.S. interagency and host-nation military health services.
The authors concur with the recommendation of the National Academy of Sciences that intentional intra- and interagency coordination and collaboration, including DOD activities, would greatly improve the government’s overall effectiveness in meeting the stated goals of international health security efforts. Protecting the nation against biological threats before they reach U.S. shores requires the combined experience and expertise resident in many government institutions, including the United States Agency for International Development (USAID), the DOD, the U.S. Department of Agriculture, and the U.S. Department of Health and Human Services—which notably contains the CDC, the Food and Drug Administration, the National Institutes of Health, and the Office of Global Affairs.
The DOD possesses some of the most comprehensive health and biosecurity capabilities in the world, yet coordination within the Department has been hampered by stovepiping due to the diffusion of responsibility and funding throughout the organization. Fortunately, since J. Christopher Daniel and Kathleen H. Hicks addressed this issue in a 2014 CSIS paper, significant progress has been made in improving collaboration and information sharing through coordinating bodies such as the DOD Global Health Engagement Council, established in 2017. Chaired by the assistant secretary of defense for special operations and low-intensity conflict, its members include the assistant secretaries for homeland defense and global security; health affairs; and nuclear, chemical, and biological defense programs. Although this is an encouraging step, more can be done to ensure that the DOD’s remarkable assets combine to combat intentional, accidental, or naturally occurring infectious disease threats.
Protecting the nation against biological threats before they reach U.S. shores requires the combined experience and expertise resident in many government institutions.
Strengthening host nations’ health systems also supports stability and improves relationships. Mutually planned, continuously funded programs that meet partner nations’ needs are the most effective. Uncertain funding and frequent personnel changes are invariably disruptive.
ALIGNMENT
NSD-1 mandates an analysis of the security implications of biological threats and an evaluation of how U.S. agencies can best support international efforts, including by adjusting funding levels. Notably, the directive focuses on the Global Health Security Agenda (GHSA), a voluntary international cooperative framework intended to strengthen all nations’ public health systems so they can effectively prevent, detect, and respond to infectious disease threats. Although the DOD is not specifically funded to support the GHSA, many capabilities directly support its tenets:
- Since World War II, Army and Navy overseas infectious disease research laboratories have worked closely with military and health ministry researchers in host nations on basic science, vaccine and therapy development, and disease surveillance.
- The Department of Defense HIV/AIDS Prevention Program (DHAPP) assists militaries in about 50 countries with culturally focused, military-specific HIV/AIDS prevention, care, and treatment programs.
- The Defense Threat Reduction Agency’s Biological Threat Reduction Program (BTRP) conducts efforts against especially dangerous pathogens, including by strengthening partner nations’ overall disease surveillance, diagnostic, and therapeutic capabilities.
- U.S. military forces routinely support international humanitarian assistance and disaster response (HADR) activities, both as part of military exercises and in real operations.
- The DOD sponsors and participates in episodic military medical conferences, exercises, and subject-matter expert exchanges on topics ranging from combat trauma and aeromedical evacuation to infectious disease. Examples include the annual Indo-Pacific Military Health Exchange and the International Committee on Military Medicine.
FUNDING
The most successful public health and infectious disease programs strengthen the medical and public health capabilities of host nations’ militaries, develop strong relationships, and create trust. This requires time and stability. However, many military health-engagement activities are one-time events carried out through Geographic Combatant Commander (GCC) security cooperation programs; these are supported with funding managed by the Defense Security Cooperation Agency, which sets specific restrictions on uses and duration. Uncertain funding can interrupt programs dependent on sequential steps, making these efforts counterproductive.
A Moment of Opportunity
The U.S. military’s broad expertise in health, biosecurity, and biosafety is not only fundamental to the readiness of U.S. troops, it also contributes substantially to interagency efforts against biological agents at home and overseas. The DOD’s exceptional strengths in logistics, planning, and lift activities were at the core of Operation Warp Speed’s success and subsequent vaccine distribution in the United States, and biological research performed in DOD organizations has proven essential to recent rapid advances in vaccine development and biological agent detection. These assets will likely play an important role in U.S. global engagement. Military experts in public health, infectious disease research, and bioterrorism should continue to expand collaboration with each other and their civilian colleagues across the many shared fields that will be required to address all biological threats to national security.
Military medical and biosecurity experts bring considerable value to civilian-led health security efforts and enhance research and capacity-building partnerships with national governments, universities, and international organizations. Long-standing international efforts such as the President’s Emergency Plan For AIDS Relief (PEPFAR) have successfully controlled disease while providing the world a positive example of U.S. civil-military collaboration.
All successful organizations evolve, and reorganization and realignment will improve coordination and increase efficiencies. However, extreme care will be necessary to avoid pushing out the dedicated, high-quality, professional members of the DOD’s clinical, public health, research, and scientific staff who are essential to the Department’s contribution to U.S. biosecurity.
None of this is easy. It requires effective leadership at the DOD and in other agencies, as well as bipartisan support in Congress. It requires forward thinking and political will to encourage collaboration over division. It requires carefully thinking through what contributions the DOD can make globally as U.S. diplomatic engagement expands to address the looming vaccine crisis and other related global health security challenges. It requires dedication to develop successful programs and to create and sustain new models that will continue to thrive under subsequent administrations. And it requires codifying the DOD’s role as a major interagency biosecurity partner in combating biological threats—be they naturally occurring, accidental, or intentional—in the 2022 National Defense Strategy and the Defense Planning/Programming Guidance.
Dr. Thomas Cullison is an adjunct fellow with the Global Health Policy Center at the Center for Strategic and International Studies (CSIS). During his 38-year naval career, culminating as deputy surgeon general of the Navy, he was active in disaster management, international health engagement, graduate medical education, and health policy. He has contributed to numerous CSIS Global Health Policy Center programs and remained active in Department of Defense contributions to health security.
Stephen Morrison is senior vice president at CSIS and director of its Global Health Policy Center. Dr. Morrison writes widely, has directed several high-level commissions, and is a frequent commentator on U.S. foreign policy, global health, Africa, and foreign assistance.
This report is a product of the CSIS Commission on Strengthening America’s Health Security, generously supported by the Bill & Melinda Gates Foundation.
This report is produced by the Center for Strategic and International Studies (CSIS), a private, tax-exempt institution focusing on international public policy issues. Its research is nonpartisan and nonproprietary. CSIS does not take specific policy positions. Accordingly, all views, positions, and conclusions expressed in this publication should be understood to be solely those of the author(s).
© 2021 by the Center for Strategic and International Studies. All rights reserved.
Please consult the PDF for references.