Bring DOD Fully into the Mix of Pandemic Preparedness and Response
Thomas R. Cullison and J. Stephen Morrison. "Bring DOD Fully into the Mix of Pandemic Preparedness and Response." CSIS Commission on Strengthening America's Health Security, Center for Strategic and International Studies, June 30, 2022. Accessed October 01, 2025. https://healthsecurity.csis.org/articles/bring-dod-fully-into-the-mix-of-pandemic-preparedness-and-response/
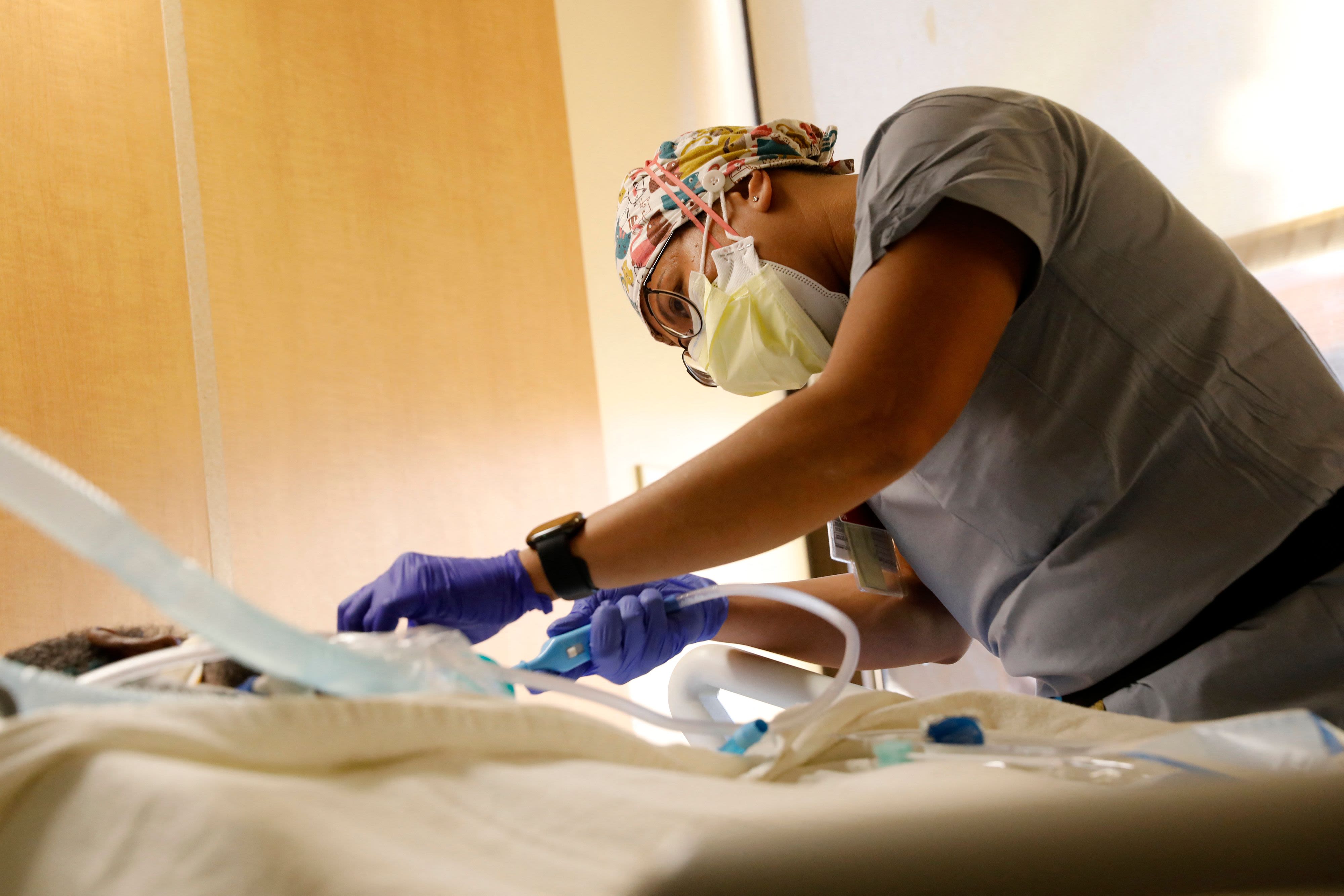
Achievements Downplayed and Obscured
Throughout the Covid-19 pandemic, the Department of Defense (DOD) has made major contributions, both domestically and internationally, to civilian-led preparedness and response, particularly in logistics and planning, and numerous biomedical arenas including research, direct clinical care, and all aspects of public health including a worldwide network of infectious disease research laboratories. Certainly, DOD will be called upon to augment civil authorities for future similar crises both at home and abroad as it has been so often in the past with Ebola, SARS, MERS, and numerous other outbreaks. Often, however, these contributions arise amid sudden emergency demands, in an ad hoc fashion, without adequate forward mission planning and budgeting, and without clear backing in U.S. national security doctrine. And often DOD actions have deliberately low visibility—they are soon out of sight, out of mind—and are neither appropriately acknowledged nor well understood.
At the recent second Global Covid-19 Summit, organized by the White House in collaboration with heads of state representing the G7, G20, African Union, and Caribbean Community (CARICOM), there was no mention of DOD’s special assets and recent performance, no DOD presence among participants, and no consideration of DOD’s current and future contributions to the global response. At some level, that omission is no surprise: the summit is first and foremost about the civilian response. At another, it is a sign of an enduring problem.
Multiple factors account for why the DOD role is so often obscured:
-
DOD is typically called upon, at short notice, to play a temporary role addressing critical, often embarrassing gaps, indeed failures, in the civilian sphere. DOD is itself hesitant and ambivalent: many within DOD do not regard its support of pandemic response as part of its core mission, even though its special expertise in intentional or accidental biological events is well recognized.
-
Medical and public health capabilities overwhelmed by a pandemic are fundamentally no different from other disasters for which militaries routinely prepare and respond, both domestically and internationally, when civilian capabilities are insufficient. Yet significant preparation and planning are regularly exercised for many likely scenarios, such as wildfires, tropical storms, and earthquakes, while the same is not true for biological events.
-
Certain live sensitivities are always at play. DOD commitments cannot be open-ended, otherwise they will compromise DOD’s core readiness and operational missions. The commitments cannot be seen, either at home or abroad, as militarizing and dominating the pandemic response. To answer these concerns, it is critically important to clarify early what the likely required capabilities are and how they will be resourced. When that step has not been taken ahead of a sudden emergency, hesitation can follow.
These many important considerations notwithstanding, DOD remaining in relative obscurity also carries a price. Often DOD’s capacities are allowed to wither after the emergency has faded, particularly if DOD is not at the interagency table—before, during, and after the crisis—to contribute in a sustained way to strategic planning for future pandemics, with adequate forward budgeting. If DOD’s special assets are not operationally integrated with other agencies, well in advance, into overall U.S. health security strategies, both at home and abroad, hesitation, ambivalence, and ad hoc decisionmaking will follow. This all contributes to high inefficiency and confusion, impeding an effective DOD role.
Spotlight Achievements
One essential step in pulling DOD out of obscurity and into the full light of day—into an open discussion of what is required to guarantee and sustain U.S. health security—is simply to continually remind policymakers and planners of DOD’s impressive record of achievement.
Logistics, Lift, and Planning. Military logistics, lift, and planning capabilities were instrumental in Operation Warp Speed’s historic success in developing and distributing safe, effective vaccines in record time: prior DOD-supported research created the mRNA vaccine platform that subsequently undergirded the accelerated development of the Pfizer and Moderna vaccines. Defense logistics experts charted the complicated end-to-end supply chain requirements for manufacture and filled critical positions in expanded manufacturing facilities until civilian replacements could be hired. The White House invoked the Defense Production Act to guarantee a single-minded focus on speeding manufacture through government-guaranteed contracts for millions of doses, in parallel with clinical trials necessary for Food and Drug Administration approval. Defense contracting experts were the only federal capability positioned to execute these contracts within the time constraints necessary to deliver vaccines in time to save lives.
Research and Development. The Department of Defense performs and supports biological and medical research primarily for the purpose of protecting the health of the armed forces. This includes the ability to prevent, detect, and treat many diseases rarely, if ever, seen in the United States, such as Ebola and malaria, as well as more generalized threats such as HIV and coronaviruses that cause diseases such as SARS, MERS, and Covid-19. But in almost all instances, the fruits of this work benefit the population as a whole. That was true in the development of diagnostics to detect anthrax spores in post offices following the 9/11 attacks, the development of almost all current antimalarial medications, and promising work on vaccines against HIV and coronaviruses, in addition to the mRNA vaccine platform mentioned above.
Public Health and Clinical Care. Early in the Covid-19 pandemic, it became clear that U.S. civilian public health and clinical capabilities were woefully insufficient and at high risk of breakdown in many of those areas hardest hit. Thousands of National Guard, reserve, and active-duty military personnel filled the breach, providing administrative, logistical, and direct clinical support. Although extremely effective, this DOD rapid support was not without a cost to military readiness. It impacted access to routine healthcare in military treatment facilities across the country. Particularly worrisome was the heavy demand for many of the same highly skilled clinical personnel, such as intensive care physicians, nurses, and technicians, who deploy with operational forces to support combat casualty care. This stress unfolded at the same time that DOD leadership weighed how to manage the congressionally mandated reduction of over 12,000 active-duty uniformed health personnel.
International Health Engagement. U.S. military international health engagement activities play a significant role in assisting partner nations to strengthen health systems in order to more fully comply with the International Health Regulations, in line with the intent and goals of the Global Health Security Agenda. Ongoing programs such as the Defense HIV/AIDS Prevention Program (closely aligned with PEPFAR) and military overseas infectious disease laboratories have for decades worked in tandem with health ministries and militaries throughout the globe. Ongoing military-to-military exercises, scientific meetings, and other partnerships develop long-standing relationships, and host nation capabilities repeatedly prove effective in real world events such as the West African Ebola outbreak and successful responses to Covid-19 by host nation activities requiring no additional U.S. support. These efforts are most effective when closely aligned with similar activities of federal agencies such as the U.S. Agency for International Development (USAID) and the U.S. Centers for Disease Control and Prevention, nongovernmental organizations, and the host nation itself.
Biosurveillance, Biosafety, and Biosecurity. DOD maintains many abilities to prevent, detect, and respond to biosecurity and biosafety lapses, whether naturally occurring, accidental, or intentional. Internally within DOD, collaboration is improving among the various organizations dealing with biological threats: specialized research laboratories, a worldwide network of overseas infectious disease research laboratories, the National Center for Medical Intelligence, the Global Emerging Infections Surveillance System (GEIS), the Biological Threat Reduction Program (BTRP), and military public health activities to mention only a few. The DOD Biodefense Posture Review currently underway aims to unify and improve defense capabilities against biological threats of any sort and better synchronize them with other federal agencies, particularly the U.S. Department of Health and Human Services (HHS) and the Federal Emergency Management Agency (FEMA) domestically, and the U.S. Department of State (DOS), USAID, and HHS overseas, in accordance with U.S. national goals and strategies.
Four Additional Steps to Strengthen DOD’s Role
-
Align Capacities. There is a need for intensified efforts to better coordinate biosecurity activities within DOD; improve alignment among external partners, including the private sector; and clearly establish in evolving doctrine that pandemic preparedness and response are matters of U.S. national security. The secretary of defense–directed Biodefense Posture Review currently underway presents an opportunity for improved collaboration and cooperation in all of these areas.
The Biden administration’s renewal of the National Security Council Directorate on Global Health Security and Biodefense strengthens the ability to more fully incorporate DOD’s many unique capabilities through partnerships across government, industry, and academia. Specifically, alignment of the upcoming National Biodefense Strategy with the National Security, Defense, and Military Strategies will go a long way toward presenting a united vision for dealing with future pandemics. Supporting policies and directives can further improve alignment of DOD capabilities with HHS and FEMA domestically and DOS, USAID, HHS, and the CDC internationally.
-
Recognize Pandemics as Disasters. Defense must be at the table from the beginning in discussions of all types of biological threats as well as other aspects of emergency preparedness and response, such as tropical storms, tsunamis, and earthquakes. The familiar disaster risk reduction cycle—preparation, response, recovery, and prevention leading once again to preparation—adapts nicely to pandemic events.
It is essential to ensure that DOD is present at the interagency table—before, during, and after pandemic crises—to be able to consistently and fairly represent the broad spectrum of DOD capabilities and interests around intentional, accidental, and naturally occurring biological events and how to effectively integrate these assets into overall preparation and response activities. Understanding the different interagency relationships for domestic and foreign events is vital if organizations are to work together in partnership toward a common goal from the beginning.
- Secure Budgets. Funding must be aligned with desired outcomes. Investing at a higher level continuously over time in biosafety and biosecurity programs will be essential in these times when those risks have risen steeply. Following the Biodefense Posture Review, a critical evaluation should commence centered on how funding is to be aligned with DOD biological programs. This is particularly important in annually providing sufficient funds for BTRP biosafety and biosecurity programs, GEIS, and the Overseas Humanitarian, Disaster, and Civic Action (OHDACA) program, as well as in creating multi-year funding support for military health engagement activities aimed at improving host nation health system strengthening.
-
Integrate Biosecurity with U.S. Strategic Interests. DOD’s health security capacities should become a much better integrated and more significant component of U.S. engagement in zones of high geopolitical consequence.
DOD can contribute much to cement the Quad partnership between the United States, Australia, India, and Japan: genetic sequencing and clinical trials; studies of vaccine efficacy and approaches to boosters; planning and executing expanded vaccine coverage; and access to therapies and testing.
DOD can make similar parallel contributions in Europe with Ukraine and NATO allies by conducting training missions on refugee medicine, combat casualty care, and humanitarian emergencies. From outside of Ukraine itself, DOD can contribute to the planning process for the strengthening of Ukraine’s military medical infrastructure.
DOD’s various forms of overseas health engagement are increasingly subject to Russian and other sustained disinformation campaigns that seek to undermine popular trust and confidence in DOD activities. DOD can and should develop more effective communications strategies to combat this expansive threat.
Clarity of Purpose Is Superior to Ambivalence and Neuralgia
The world is far from done with Covid-19. The evolving virus still rules, amid high uncertainty. Civilian capacities will continue to improve but also continue to lag behind what is required during periods of shock. DOD’s role will remain vitally important as the United States weighs its future approaches at home and abroad. DOD will make a far superior contribution if its pandemic contributions are endorsed in doctrine, better aligned internally and externally, and better understood and acknowledged by policymakers and American citizens, and if DOD actively participates at the interagency planning table and enjoys reliable and adequate long-term financing. Showing what DOD can do in geopolitical zones of high consequence should be a high priority.
Thomas R. Cullison is a senior associate (non-resident) with the Global Health Policy Center at the Center for Strategic and International Studies (CSIS) in Washington, D.C. J. Stephen Morrison is senior vice president and director of the CSIS Global Health Policy Center.
The authors gratefully thank several individuals who generously shared their expertise in the development of this commentary, including Vice Admiral Raquel Bono, Amb. Mark Dybul, Thomas R. Frieden, Margaret “Peggy” Hamburg, Amb. Karl Hofmann, Amb. Jimmy Kolker, Hon. Deborah Rosenblum, and Hon. Juan Zarate, among others. These individuals contributed to the commentary in their individual capacity, not as representatives of their respective organizations, and language included in this commentary does not imply institutional endorsement by the organizations that participants represent. This is not a consensus document and the opinions expressed are the sole responsibility of the authors.
Commentary is produced by the Center for Strategic and International Studies (CSIS), a private, tax-exempt institution focusing on international public policy issues. Its research is nonpartisan and nonproprietary. CSIS does not take specific policy positions. Accordingly, all views, positions, and conclusions expressed in this publication should be understood to be solely those of the author(s).
© 2022 by the Center for Strategic and International Studies. All rights reserved.