North Kivu’s Ebola Outbreak at Day 90: What Is to Be Done?
J. Stephen Morrison and Judd Devermont. "North Kivu’s Ebola Outbreak at Day 90: What Is to Be Done?." CSIS Commission on Strengthening America's Health Security, Center for Strategic and International Studies, November 02, 2018. Accessed October 01, 2025. https://healthsecurity.csis.org/articles/north-kivu-s-ebola-outbreak-at-day-90-what-is-to-be-done/

The Issue
There is a high risk that the international response to the Ebola outbreak in eastern Democratic Republic of the Congo (DRC), the first in a war zone, is falling far short of what is required. Indeed, we may be at the edge of a swiftly expanding epidemic that spreads regionally and perhaps beyond. Armed attacks, wary communities, and insufficient on-the-ground capacity are major barriers to arresting the outbreak. There is an urgent need for high-level political attention focused on generating an updated game plan to improve security, train and deploy community health workers and Congolese public health experts, and win community trust and cooperation. The United States—vitally important to the international response in West Africa 2014-2016—has chosen thus far, out of security concerns, to limit its engagement to the periphery of the outbreak. Quick action is needed to affirm U.S. leadership in eastern Congo, better understand the specific security threats at play, and come up with practical solutions that permit the safe deployment of a small U.S. expert contingent into the center of the outbreak, where seasoned U.S. talent is most needed.
Introduction
In the third week of October, armed rebels in two separate attacks killed 19 individuals in two separate attacks in the vicinity of the major urban center of Beni and kidnapped a dozen children. This was the most recent of multiple deadly attacks since the Democratic Republic of the Congo (DRC) announced an Ebola outbreak on August 1 in the populous, perennially violent and chaotic North Kivu province of eastern DRC. Ironically, the attack immediately followed the Emergency Committee of the World Health Organization (WHO) ruling that the outbreak did not yet constitute a Public Health Emergency of International Concern (PHEIC).
Many health security crises today appear in fragile or broken states, ungoverned territories, and areas of open conflict. The Ebola outbreak unfolding in North Kivu and Ituri provinces is the most recent, powerful showcase of what it means to battle dangerous health security threats in a disordered world.
Rising apprehension and uncertainty surround the international response to what is now unfolding in the DRC, the first Ebola outbreak in an active war zone. While categoric judgments are elusive, it is nonetheless becoming more and more apparent that there is a high risk of losing the game in the DRC, resulting in a break-out epidemic.
On-the-ground Congolese capacity is insufficient, both trained community workers and professional public health expertise. The response is also weakened by the conspicuous absence of seasoned U.S. experts at the epicenter (along with insufficient numbers of other international experts). Armed attacks have repeatedly convulsed the response, undermining essential activities such as contact identification and monitoring; in the meantime, the threat of future attacks persists. Community trust in health personnel, the essential element in winning cooperation, is sorely lacking, translating in many instances into active resistance. As a result of these multiple barriers, responders have not yet reliably and steadily arrested the outbreak. Indeed, they are falling short in their efforts to break transmission through rapid identification, isolation, and treatment of Ebola cases; target vaccinations of all who need them; trace all contacts; and ensure safe and dignified burials.
Rising apprehension and uncertainty surround the international response to what is now unfolding in the DRC, the first Ebola outbreak in an active war zone . . . there is a high risk of losing the game in the DRC, resulting in a break-out epidemic.
More than 90 days into this dangerous outbreak, there is an urgent need to reassess. Determined high-level engagement is needed to devise realistic solutions that can stop attacks, win over wary communities, and strengthen the ground game. U.S. leadership remains essential across all fronts.
A Promising Start
The Congolese and international mobilization into the outbreak zone has been quick and laudable.
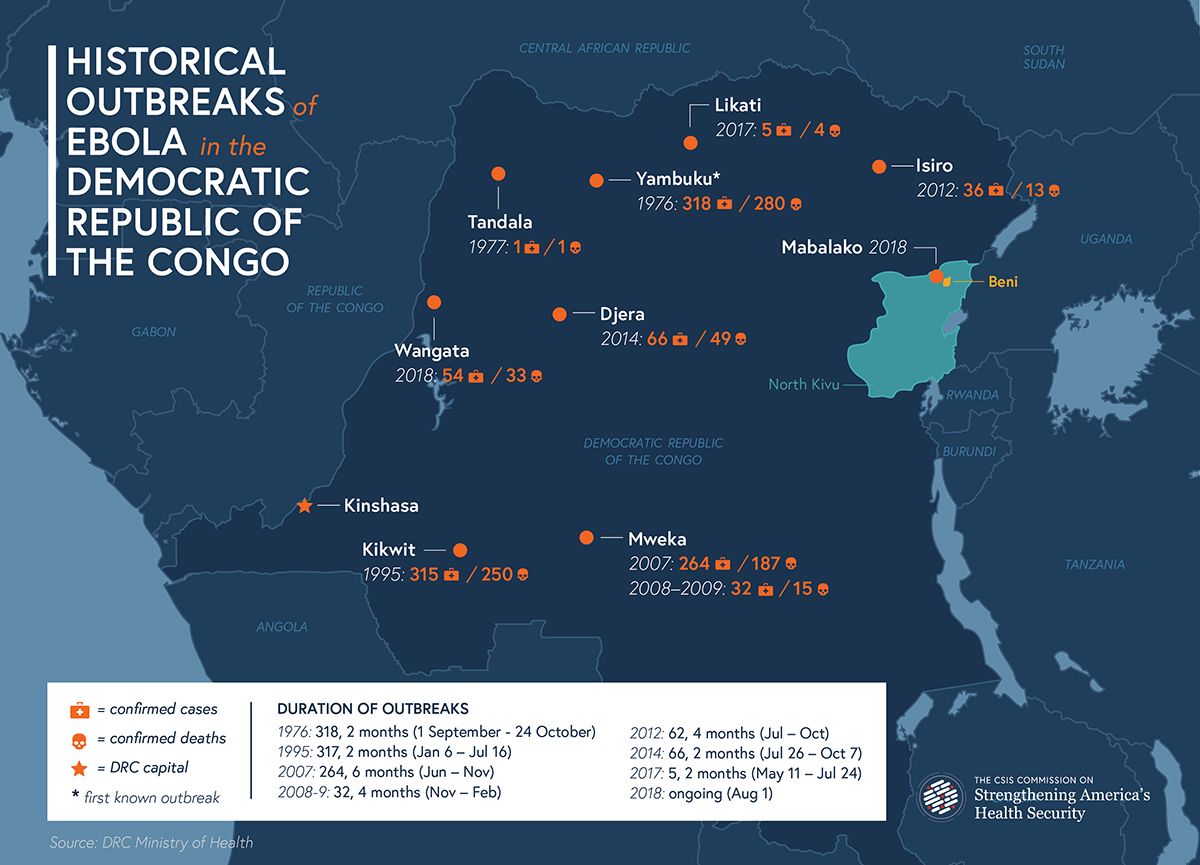
The WHO, the DRC Ministry of Health, Doctors without Borders (MSF), the International Federation of the Red Cross/Red Crescent, and key international NGOs such as the International Medical Corps have deployed, in aggregate, over 500 personnel. It is important to recall that the DRC, by contrast with Liberia, Sierra Leone, and Guinea, has successfully contained nine Ebola outbreaks, including one that surfaced in May 2018 in Equateur province.
Facilities supported by International Medical Corps’ (IMC) emergency response team have screened more than 70,000 people, and IMC has trained over 200 healthcare workers. The International Rescue Committee is operating in and around Beni on infection prevention and control. The Rwandan and Ugandan governments are screening thousands of people crossing their borders with DRC.
Thus far, money has not been a serious constraining factor.
By contrast with the West Africa outbreak, a vaccine has been available, and thus far over 24,000 exposed or vulnerable individuals have been immunized. Patients are receiving five experimental therapies, made available under compassionate use authorities. The foundation is in place to carry out surveillance and integrate data, conduct case investigation and contact tracing, isolate and treat those sick with Ebola, and promote safe and dignified burials.
The UN peacekeeping force—the United Nations Organization Mission in Democratic Republic of the Congo (MONUSCO)—has provided security escorts on the roads leading in and out of the urban center of Beni. To date, no international or civilian national health provider has been injured or killed. (Two DRC military medical personnel were among those killed October 21. Separately, two local staff of an International Federation of the Red Cross safe burial team were recently seriously injured by community members.)
Insecurity, Demographics, Elections, Mistrust
Yet to the increased dismay of those many committed individuals leading the Ebola response on-the-ground, that effort has run headlong into a plethora of complex barriers and vulnerabilities.
Armed attacks persist, with impunity. The Allied Democratic Forces (ADF) is responsible for repeated attacks on DRC military forces in and around Beni. Each has had a concussive impact, intensifying the environment of fear and seriously disrupting the response effort. There have also been local attacks by eastern Congo’s armed, community-based Mai-Mai militias. As long as ADF and other attacks continue, the response effort will remain vulnerable to debilitating setbacks.
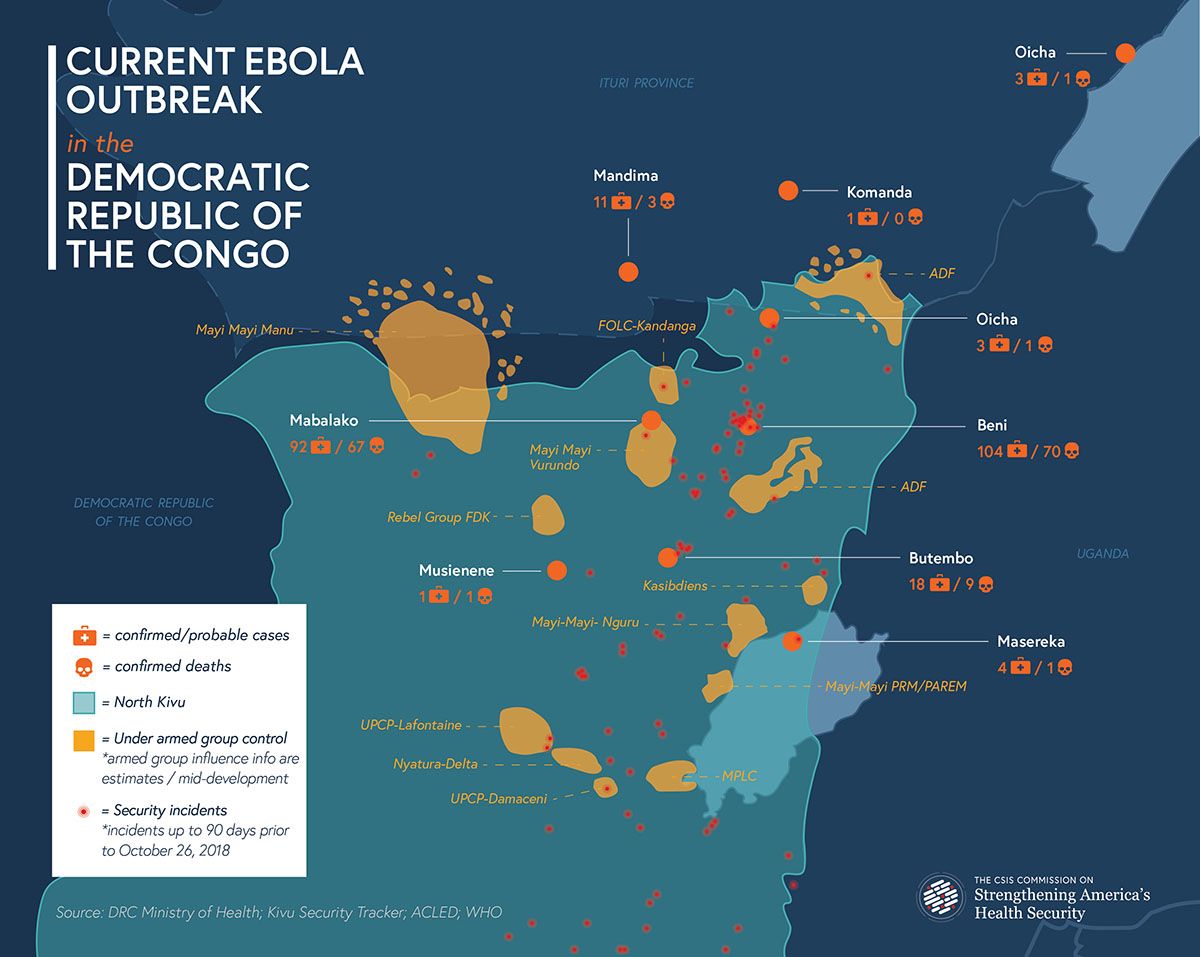
These attacks emerge within what WHO has described as North Kivu and Ituri’s “perfect storm”— over 40 armed groups, potentially destabilizing elections, and a large, highly mobile population in close proximity to porous, international borders. Its population for years has lived through recurrent humanitarian emergencies. The DRC national government, located a thousand miles away in Kinshasa, has never truly gained effective control or legitimacy in the east. While criminal groups, Mai-Mai militias, and the rebel ADF are credited with the majority of the violence, the DRC’s security forces have an equally infamous reputation; since 2017 they have killed over 100 civilians in North Kivu.
Yet to the increased dismay of those many committed individuals leading the Ebola response on-the-ground, that effort has run headlong into a plethora of complex barriers and vulnerabilities.
Presidential, regional, and legislative elections stand on the horizon, scheduled for December 23, 2018. In the midst of the current Ebola outbreak, that could be a source of major distraction, on the part of national leadership. It could also exacerbate tensions in the east, compounding, in turn, the odds of getting control over the epidemic.
In 2014, Liberia repeatedly delayed its senatorial elections for two months because of fears around public gathering during the Ebola crisis. If President Kabila were to do the same and postpone the election in the DRC, even in part, it could fuel significant unrest because Kabila is deeply unpopular, and any adjustment to the election schedule would confirm suspicions that Kabila has no intention to step down after 17 years in power. Kabila is especially unpopular in eastern Congo where anti-government protests are a common occurrence in Beni and Goma. If elections hold, past experience suggests that traveling to polling stations will add to cross-regional migration flows and may increase transmission.
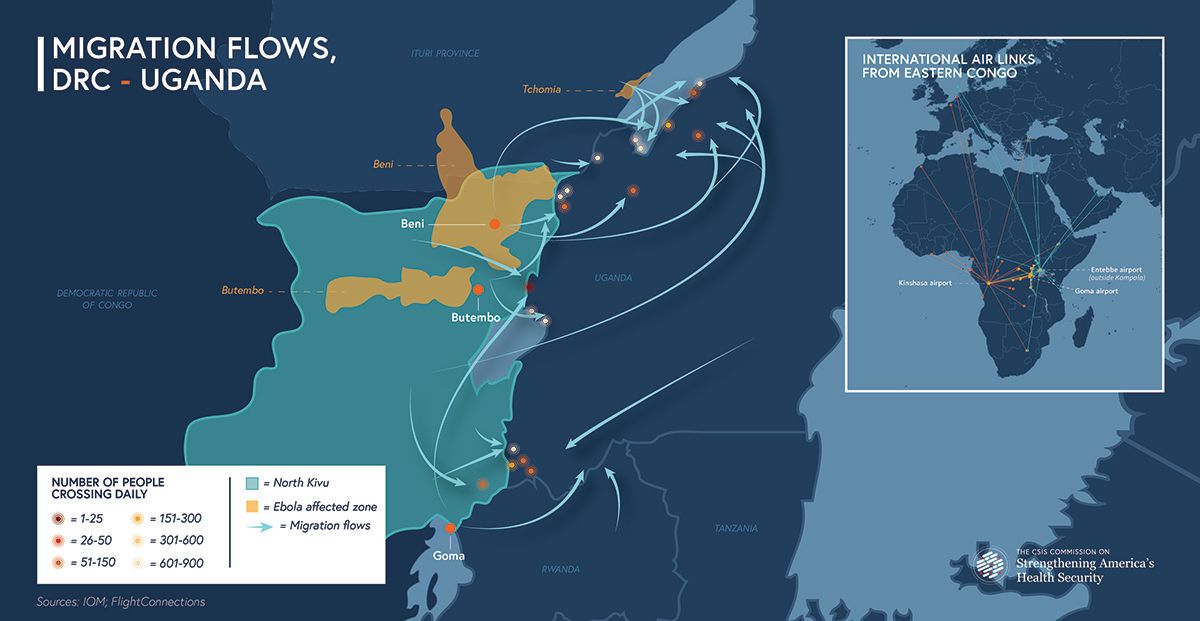
The region’s demographics are daunting, both for getting control over the outbreak and containing its spread beyond. There are 6 million people living in North Kivu, making it nearly 1.5 times denser than Guinea, Liberia, and Sierra Leone combined. Of North Kivu’s population, 1.1 million are internally displaced. Tens of thousands of traders, refugees, internally displaced persons, and militants circulate through the region and into neighboring states daily, increasing the likelihood of a widening transmission. The urban epicenter, Beni, is just 300 miles away from Uganda’s capital, Kampala, an international transit hub.
The lack of trust and engagement with communities is a critical barrier, as well as insufficient local capacity to manage the outbreak. As seen in West Africa in 2014-2015, there is active community resistance to responders: hostility and mistrust, refusal to cooperate in identifying cases and persons who have been exposed, including deliberate misreporting, and obstruction of safe and dignified burials. These same communities face a critical shortage of skilled case investigators with adequate supervision and guidance.
After decades of government repression and ineffective international responses, civilians, not surprisingly, often regard response efforts with considerable suspicion. Anthropologists deployed with the Congolese Ministry of Health report that the government is “not doing enough to make it safe. The United Nations is judged to be complicit in the massacres here, and for not protecting the population except for a few battalions. And NGOs, people think they are here just to make money.” Rumors circulate that Ebola is “witchcraft,” a government tactic to stall elections or even a ploy introduced by the international community.
There are limits to the security protection MONUSCO can offer. Local Congolese view the United Nations as compromised by its association with the DRC national government and its security forces. To preserve their neutrality, groups like MSF and the International Committee of the Red Cross will not travel with MONUSCO motorcades.
Dangerous Gaps Emerging As the Ground Game Falters
The daily rate of new Ebola cases has more than doubled in early October, and an October 18 WHO bulletin indicates even this large spike may be an underestimation, indicating that “the rising trends are likely underestimated given expected delays in case reporting, the ongoing detection of sporadic cases, and security concerns which limit contact tracing and investigation of alerts.” Most experts attribute this spike in part to the temporary suspension of Ebola response programming in late September. On September 22, an attack in Beni, one of the epicenters of the outbreak, killed 21 civilians and prompted a five-day period of mourning that interrupted contact-tracing and led the rate of Ebola cases to almost double.
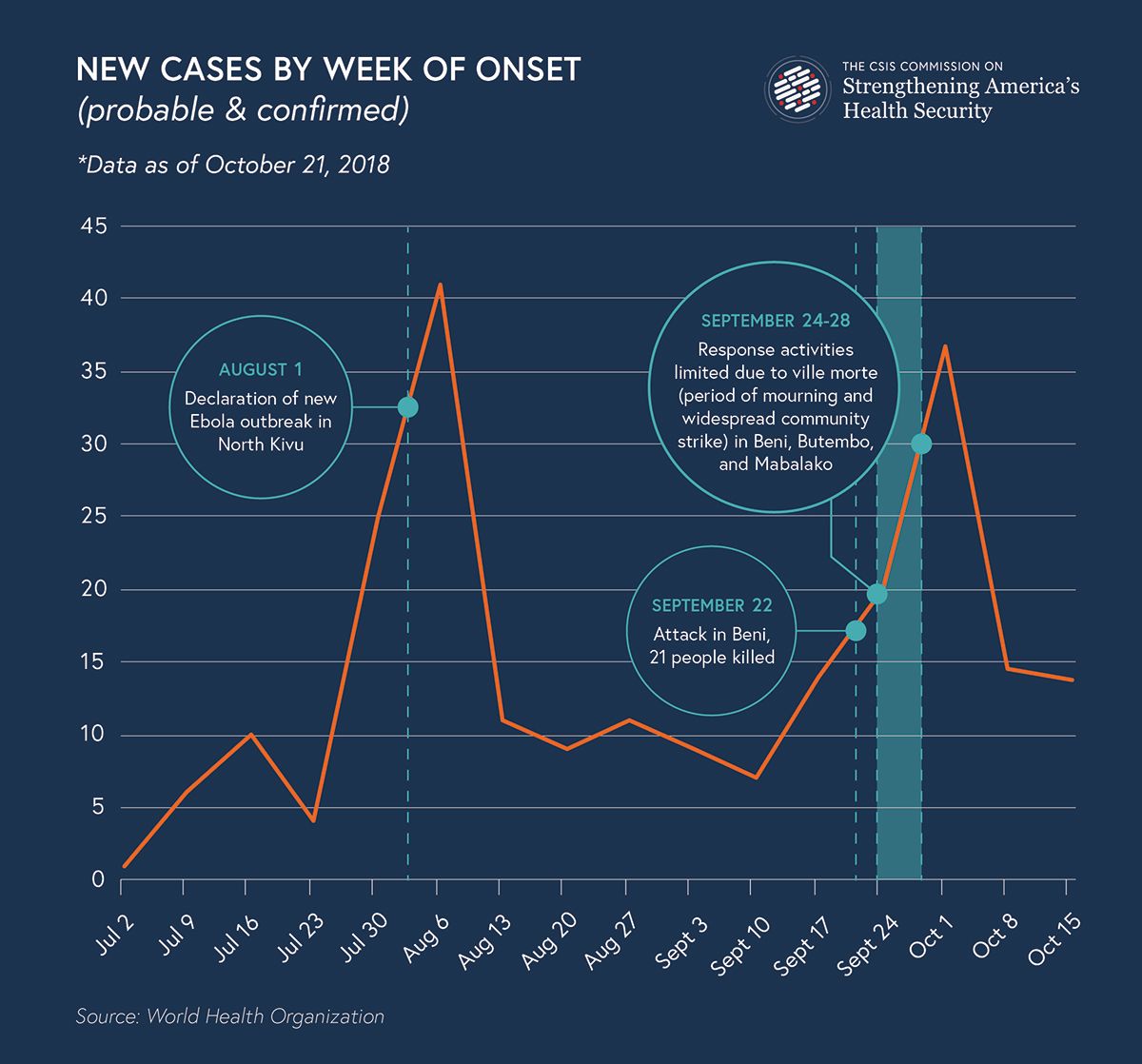
Even with the resumption of activities after the forced halt, responders remain skeptical as to whether the current effort will be sufficient to control the outbreak: they lack sufficient visibility into the origins of new cases or adequate ability to trace contacts and identify cases effectively. Emerging signs suggest there are dangerous gaps emerging that invite the expansion—not the arrest—of the outbreak. Cases are on the rise, including secondary transmission within communities, while the knowledge of where they originate, and with whom these ill individuals have come in contact, is deteriorating. The time lapse between identifying symptomatic cases and isolating and treating them remains dangerously large.
Prevention and control of infection have been highly problematic. Numerous cases have been missed by triage, and there are clear signs of transmission in both NGO and public health facilities: 25 health workers have been infected with Ebola, of whom three have died. Beni Hospital has been described as “abysmal” in its controls.
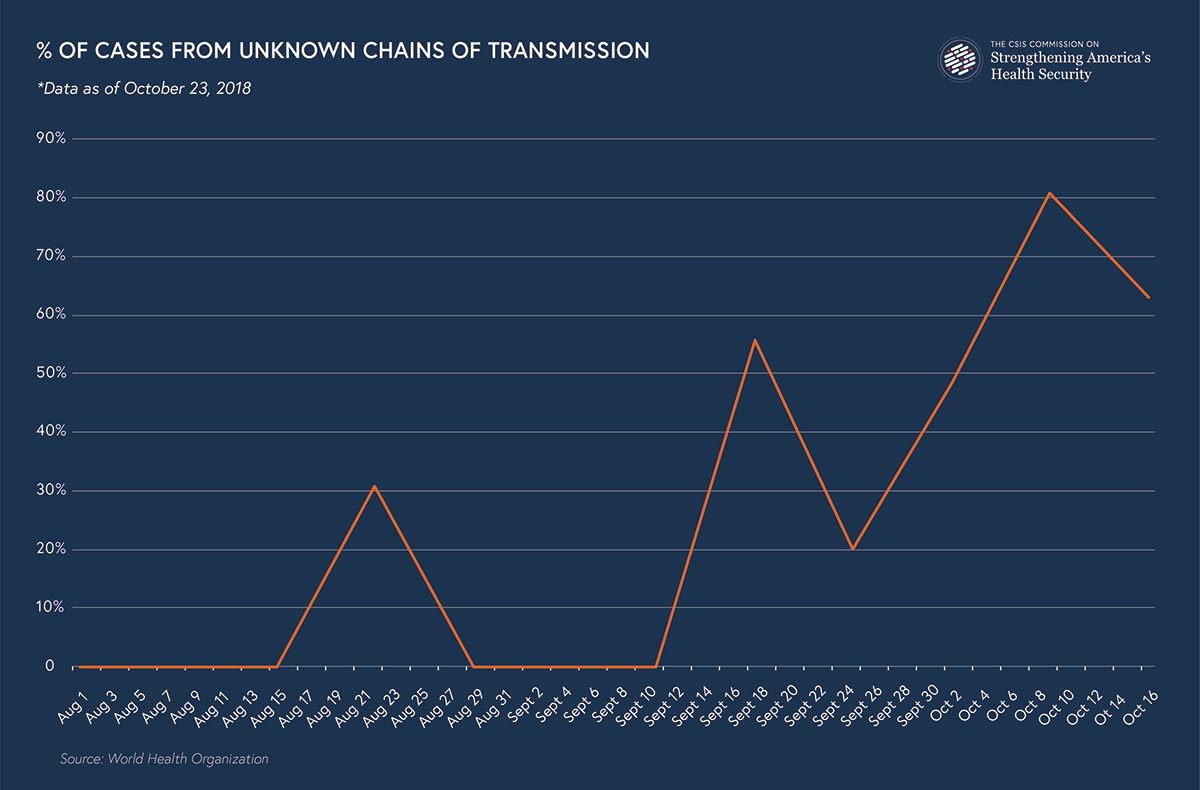
The proportion of new confirmed cases, which do not appear on any contact list and have no known epidemiological link to prior cases, has risen in recent weeks to roughly 60 percent to 80 percent. That means, in effect, that contact tracing is only covering 20 percent to 40 percent of actual contacts. Responders are operating in the dark on the balance of contacts.
The monitoring of known contacts—intended to be twice daily communication for 21 days—has also proven problematic, as follow-up has faltered and cases have been lost. The WHO reported on October 17 that contact tracing performance in the previous week ranged from 52 percent to 87 percent, attributing this poor performance to the challenges of contact tracing in restive Beni. There is no cumulative record at present of the numbers and identities of those contacts who have gone missing.
U.S. Policy Caught in a Bind
The Ebola outbreak in eastern Congo occurred just a few months after the decision by the Trump administration in May to dismiss Rear Admiral Tim Ziemer and dissolve his post as senior director for global health security and biothreats at the National Security Council. That downgrading of health security at the White House raised questions of how well-equipped the administration would be in the future to manage dangerous outbreaks.
One factor contributing to weaknesses in the international ground response is the decision thus far by the United States to keep its seasoned civilian experts—essential players in prior Ebola outbreaks—at a distance from the conflict zone, out of harm’s way.
This caution reflects the grave—and undeniable—security threats in eastern Congo. It may also reflect President Trump’s own personal skepticism about the wisdom of the United States leading an international response, given his prior vociferous objections —through Twitter and elsewhere —to the U.S. engagement in West Africa in 2014.
Such caution is also contrary to the fundamental lesson learned in the West African Ebola outbreak in 2014-2015: attack the outbreak quickly at its source. In the DRC case, this decision has held back critically important, seasoned Centers for Disease Control and Prevention (CDC) expertise in surveillance and data integration, community relations, case investigation and contact tracing, and safe and dignified burials. In the Ebola outbreak in West Africa in 2014-2015, over 1,400 CDC personnel voluntarily did rotations. None were seriously injured or infected during the response, despite often quite adverse conditions.
One factor contributing to weaknesses in the international ground response is the decision thus far by the United States to keep its seasoned civilian experts—essential players in prior Ebola outbreaks—at a distance from the conflict zone, out of harm’s way
Only a few U.S. personnel have been on the ground in Beni for a very brief period. Three staff from CDC and one staff from the United States Agency for International Development (USAID) were deployed to Beni on August 22. Two days later, the ADF attacked a DRC military base located on a road traveled by U.S. personnel. Due to security concerns, the four U.S. staff were pulled back to Goma and were not cleared to return to Beni.
Over the subsequent two months, an unresolved debate has unfolded within U.S. interagency circles over what the policy approach should be, including security preconditions, for redeploying U.S. civilian personnel into Beni and its environs. At present, the United States provides technical support to the health ministry in Kinshasa, while providing similar assistance to Rwanda, South Sudan, and Uganda for surveillance, infection prevention and control, border screening, and emergency management. CDC also provides staff to support WHO in Geneva and USAID has hired three contractors to support WHO in the outbreak zone, in non-supervisory roles.
CDC Director Robert Redfield on October 23 disclosed that he had pressed for U.S. experts to work at the epicenter of the outbreak, on public health grounds. In his view, the absence of U.S. personnel on the ground is undermining the international response: there is “an enormous disadvantage of not having expertise the CDC has on the ground.” Up to now, security considerations have prevailed. The U.S. government’s risk aversion sends a strong message to the international community that the security risks are too high to warrant engagement, which may, in turn, dissuade other foreign governments from deploying health experts.
Washington appears to be stalemated, caught, at least for now, in a bind. It faces the risk of deploying U.S. personnel into the center of the outbreak, where they might find themselves at the wrong place at the wrong time or be targeted violently, potentially inciting allegations in Congress, the media and elsewhere, reminiscent of Benghazi, that the Trump administration has risked U.S. lives. At the same time, the administration faces the risk that if it chooses to stay on the sidelines, and the outbreak mushrooms and globalizes, the blame will be laid at least in part at Washington’s door. There is also the possibility that President Trump may choose to become directly engaged.
What Is to Be Done?
For now, the outbreak shows no signs of abating. Arresting it could require a year or longer, in the opinion of senior U.S. officials. In the coming months, the outbreak will likely continue to churn and expand in eastern Congo. It is still unknown whether—or when—it will jump into the surrounding provinces and beyond, becoming a far more active and visible threat, regionally, and globally. In the meantime, however, fear of a widening outbreak is steadily growing among experts. WHO just recently reclassified the risk of spread to neighboring countries as “very high.” On October 30, the UN Security Council passed resolution 2439, voicing “serious concern” over the deteriorating security situation impeding the response to the Ebola outbreak in eastern Congo, “demanded” that all armed groups respect international humanitarian law and called for heightened international engagement and an expanded UN response.
Ebola in eastern DRC poses big, new, fundamental questions for which we do not yet have ready answers.
When an outbreak occurs in an active war zone, it demands a different level of security thinking: how is risk to be estimated, how much risk is acceptable, and how is risk to be managed effectively? The security challenges now appear bigger than WHO, the DRC Ministry of Health, and other partners can handle. So realistically, what more needs to happen, and what additional capacities are possible?
A second vital question is how much does the threat of an Ebola outbreak in eastern Congo, in a war zone, matter to major powers?
That question has gained considerable potency, given how much the world has changed since the West Africa outbreak of 2014-2016. In an era of rising populist nationalism in Washington, Europe and elsewhere, there is open skepticism of multilateralism. It is altogether unclear how global health insecurity ranks today, when set against North Korea and Iran; Brexit and uncertainty over the future of the European Union; and intensified geopolitical confrontation among Washington, Beijing, and Moscow.
The most urgently needed step is to focus high-level political attention on generating an updated game plan to improve security, strengthen local response capacities, and build trust and engagement with communities. Part of that effort has to be getting a more granular and real-time estimation of the security situation. Part also has to argue, forcefully and overtly, that there is simply no choice but to pursue an aggressive strategy to mitigate the security threats in eastern Congo: given the public health needs there, given how dangerous the outbreak is becoming, and given how much worse it could suddenly become.
Reportedly plans are in the works for a high-level mission, led by WHO Director-General Tedros, to eastern Congo, that might bring into focused deliberations the office of UN Peacekeeping, the DRC security and health leadership, and others. Delegations of this kind, especially if they include representatives of the UN Security Council and leadership of the African Union, can change the discourse, generate a concrete plan of action, put options before the UN Security Council and the African Union, and be the basis for appeals to the United States and other countries able to contribute financing, public health and security personnel, security equipment, intelligence sharing, and communications.
One potential solution to provide better security against major armed attacks by ADF may lie with the Force Intervention Brigade (FIB), a special sub-unit within MONUSCO comprised of 3,000 UN peacekeepers. Its current mandate is to neutralize and disarm rebel groups. This unit had remarkable success when initially deployed in 2013 to dislodge M23 rebels from Goma. The FIB has faced significant challenges in recent years, prompting UN Secretary General Antonio Guterres’ to call for its reconfiguration and a reduction of its troops. The UN Security Council might instead narrow the geographic scope of the FIB’s mandate to the Ebola-affected regions and amend its mission to safeguarding the public health response.
Winning the trust and cooperation of wary communities requires a unified, far better-resourced and coordinated campaign. A central focus should be expanded outreach, including training of local community members, creating a far greater capacity to prevent and control infection. Any such strategy would also need to prioritize winning the allegiance of the leaders of churches, civil society organizations, and trade and cultural associations—the de facto moral authorities governing North Kivu. That will likely require strengthened consultative mechanisms and the rapid provision of a broad package of highly visible health, humanitarian, and developmental benefits that meet felt needs.
To strengthen the overall quality and capacity of the public health response, the United States and others should give priority to the expanded deployment—with additional training, payment, and security support—of Congolese public health experts. This would build upon the existing core of seasoned Congolese experts who understand the Congolese environment. Many were trained under the CDC Field Epidemiology and Laboratory Training Program (FETLP), and many distinguished themselves in service in Guinea 2014-2016.
For the United States, a few discrete steps would go a long way to buoying the international response: issue a public declaration affirming that a full U.S. commitment to the outbreak response is squarely in the U.S. national interests; define quickly how many CDC and USAID experts are needed in the epicenter, and how they might be most effectively and safely deployed; and quickly assess how best to ensure the security of a small US contingent. The latter might involve embedding U.S. security personnel in MONUSCO.
For the United States, a few discrete steps would go a long way to buoying the international response.
Progress along all of these far-flung fronts will be difficult, but practical solutions still lie within reach.
This article was first published as a CSIS Brief on November 1, 2018.