Universal Health Coverage and Primary Health Care within the Covid-19 Context
Katherine Bliss. "Universal Health Coverage and Primary Health Care within the Covid-19 Context." CSIS Commission on Strengthening America's Health Security, Center for Strategic and International Studies, December 11, 2020. Accessed October 01, 2025. https://healthsecurity.csis.org/articles/universal-health-coverage-and-primary-health-care-within-the-covid-19-context/
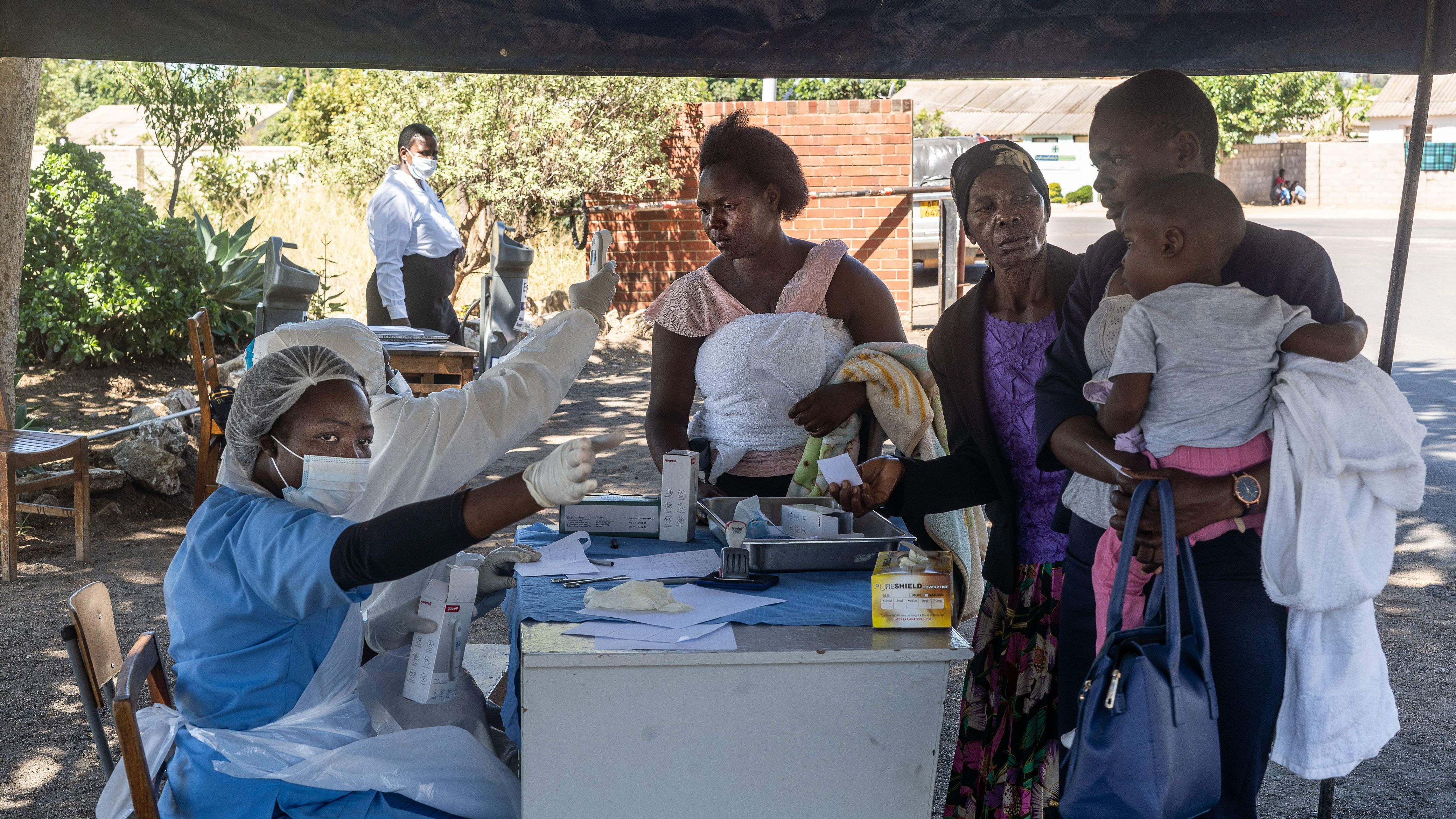
Nearly a year into the Covid-19 pandemic, as the world marks International Universal Health Coverage Day on December 12, ensuring widespread access to essential services has gained new visibility as a critical global health priority. With more than 68 million confirmed cases and at least 1.5 million deaths globally due to Covid-19, primary care clinics and providers are on the front lines of educating patients about the virus, diagnosing Covid-19 cases, and maintaining essential services in the midst of the ongoing outbreak. The theme of this year’s commemoration, “Health for All: Protect Everyone,” embodies the goals of preventing disease and ensuring the sector’s resilience in the face of an unprecedented global health crisis.
Q1: What is universal health coverage?
A1: Since the last quarter of the twentieth century, the concept of universal health coverage (UHC) has evolved from a narrow focus on primary health care services to an emphasis on improving access to a set of basic services while incorporating a newer emphasis on reducing the risk of catastrophic health expenditures. According to the World Health Organization (WHO), UHC means “all people have access to the health services they need (prevention, promotion, treatment, rehabilitation, and palliative care) without the risk of financial hardship when paying for them.”
Within the 2015 UN Sustainable Development Goals, target 3.8 emphasizes the importance of achieving universal health coverage, including “financial risk protection, access to quality essential health-care services and access to safe, effective, quality and affordable essential medicines and vaccines for all.” The UHC framework defines essential services as those related to child health, reproductive health, malaria, tuberculosis, HIV, and noncommunicable diseases, as well as mental health. In practice, this translates to a prioritization of preventive services, such as immunizations and regular checkups, and the provision of high-quality care by well-trained personnel to safeguard peoples’ health and protect them from sliding into poverty because of unexpected medical expenses. Countries’ progress toward UHC is tracked through the Service Coverage Index, which uses household and other survey data to measure peoples’ access to the set of essential services.
[

Q2: What is primary health care within the UHC concept?
A2: The 2019 global monitoring report on UHC recognized primary health care as the “route to universal health coverage,” both because services are rooted within community networks and local relationships of trust and because they offer the potential for serving as an integrated platform to deliver multiple services, including immunizations, family planning, nutrition, and care for noncommunicable diseases. This recognition builds on the 2018 Declaration of Astana, which highlighted the importance of primary health care in the quest to secure “health for all” and acknowledges the critical role primary services play in promoting health security by detecting and responding to disease outbreaks.
While there had been some notable progress in lower-income countries, where a greater percentage of the population can access interventions for infectious diseases and maternal and child health services than in the past, the 2019 report showed that there had been less improvement in access to noncommunicable diseases services since 2015. And in many countries, population growth threatened to negate recent coverage expansion. At the same time, in countries where service coverage gains had been recorded, they had frequently come at the expense of financial stability, with families spending even more of the household budget on health care than before.
Thus, in 2019, on the eve of the Covid-19 pandemic, the proportion of the global population at risk of falling into poverty because of health care expenditures was already growing. And with an estimated 70-100 million people expected to slip into extreme poverty by the end of 2021, the outlook for protecting the most vulnerable groups from further catastrophic health expenditures as the world responds to, and attempts to recover from, the pandemic is concerning.
Q3: What is the role of primary health care in responding to the Covid-19 pandemic?
A3: Over the past 11 months, the important role played by primary health care providers in responding to the novel coronavirus has become clear. Educating, diagnosing, and treating people at the community level provides a more efficient and effective approach to outbreak control than requiring them travel to distant clinics or hospitals for service.
Recognizing this fact, last spring, as the outbreak’s magnitude became apparent, global health partnerships, such as the Global Fund to Fight AIDS, Tuberculosis, and Malaria and Gavi, the Vaccine Alliance, authorized eligible countries to divert or reprogram a portion of the health systems strengthening resources they receive to outbreak preparedness and response activities, including retrofitting clinics to ensure adequate social distancing, adding new handwashing stations, and providing personal protective gear for health care workers.
In addition, the Access to Covid-19 Tools (ACT) Accelerator launched by governments, multilateral agencies, and non-governmental organizations last April to ensure all countries, regardless of income classification, can access new diagnostic, treatment, and prevention technologies, devotes an entire pillar of work to health systems. Called the health systems connector, it is overseen by the Global Fund and the World Bank and meant to streamline the delivery of lab results, oxygen, protective gear, and ensure “vital tools reach the people who need them the most.”
To promote the continuity of routine services for populations unwilling to visit clinics out of fear of being infected with coronavirus, innovative approaches to service delivery, including the increased use of telemedicine, have been effectively deployed for routine checkups, to deliver mental health services, and to manage chronic conditions that might make it particularly risky for vulnerable people to come to a health facility.
Q4: How can strong primary health care services facilitate the rollout of Covid-19 vaccines?
A4: Recent research underscores the importance of community engagement and trusted relationships with health care providers to the success of routine immunization programs as well as vaccine clinical trials and campaigns. By delivering high-quality care at the local level, primary health care facilities can serve as anchors for integrating the delivery of immunizations with other services, with care providers providing the counseling and education necessary to help patients make informed decisions about vaccinations within the context of their overall health care.
With estimates that immunization coverage rates began to decrease the spring, as families delayed checkups and well-child visits and as health workers and resources were diverted to the Covid-19 response, the WHO provided guidance to help countries maintain services or get back on track. Ensuring the sustained delivery of routine immunizations while preparing for Covid-19 vaccines can help protect child health and prevent outbreaks of vaccine-preventable disease, such as measles or influenza, from adding additional burdens to the health sector. At the same time, the distribution of Covid-19 vaccines will require a foundation of strong immunization and primary health care services in order to reach the most vulnerable populations and ensure their access to critical preventive care.
Katherine E. Bliss is a senior fellow with the Global Health Policy Center at the Center for Strategic and International Studies in Washington, D.C.
This Critical Questions is made possible with the generous support from Bill & Melinda Gates Foundation.
Critical Questions is produced by the Center for Strategic and International Studies (CSIS), a private, tax-exempt institution focusing on international public policy issues. Its research is nonpartisan and nonproprietary. CSIS does not take specific policy positions. Accordingly, all views, positions, and conclusions expressed in this publication should be understood to be solely those of the author(s).
© 2020 by the Center for Strategic and International Studies. All rights reserved.